CB2 Receptor Agonists to Restore Cytokine Balance?
Non-Psychoactive Cannabinoid Compounds to the Rescue?
I wrote earlier that the cytokine balance in Long Covid is disturbed, and that low levels of the IL-4 and IL-10 might be contributing to disease, while high levels of inflammatory cytokines seen in long haulers might also be part of the problem. And I am not surprised to find that activating cannabinoid receptors can boost levels of IL-4 and IL-10. And it doesn’t have to involve marijuana; THC works, but so do some non-psychoactive plants (and no, I’m not talking about CBD).
“Improved cognition impairment by activating cannabinoid receptor type 2: Modulating CREB/BDNF expression and impeding TLR-4/NFκBp65/M1 microglia signaling pathway in D-galactose-injected ovariectomized rats.” PLoS One, 29 Mar 2022, PMID 35349580.
The cannabinoid receptor type 2 (CBR2) is found in cells across the body, particularly cells tied to the immune system. The type 1 receptors are found in nerves, and activating the cannabinoid receptors on nerves can cause euphoria and (at higher levels), discombobulation. Activating the CB2 receptor does not have any noticeable psychoactivity, but it does reduce inflammation in a variety of ways.
This study used an experimental compound called AM1241. This molecule has been shown to activate the CB2 receptor, but not the CB1 receptor (and it does not seem to have major effects on any other known receptors). So AM1241 provides a tool to see what happens when only the CB2 receptors fire faster.
In this study, treatment with AMA1241 caused inflammation to go down, it made IL-4 and IL-10 levels go up, and cognition improved. All of these outcomes are what we want for long covid. We don’t know for sure that activating the CB2 receptor in long haulers will do this, but there is good reason to think it might. And biohackers are not limited to AM1241; there are a variety of plant compounds that selectively activate the CB2 receptor, and which have established use.
Another study found similar increases in IL-4 and IL-10 when a CB2 receptor agonist was administered in a mouse model:
“Cannabinoid 2 receptor attenuates inflammation during skin wound healing by inhibiting M1 macrophages rather than activating M2 macrophages.” Journal of Inflammation, 4 Dec, 2018, PMID 30534003.
Cannabinoid Compounds
THC is the most famous (or infamous) cannabinoid. But not the only one. A common idea is that THC in cannabis activates the CB1 receptors, while CBD activates the CB2 receptors. This idea is incorrect. THC activates both types of receptors, while CBD does not directly act on either type of receptor. CBD has an indirect effect on the cannabinoid receptors, and it activates some serotonin receptors. While CBD does have a variety of anti-inflammatory properties and may be useful for a condition like long covid, we cannot assume that it works through the same mechanism as AM1241.
While the plant Cannabis sativa is the only plant known to produce THC and CBD, it is far from the only plant that produces molecules that tickle the cannabinoid receptors. Kava produces a molecule called yangonin, and it (like THC) hits the CB1 receptor and produces relaxation and euphoria. 1 Lemon balm and many other herbs contain rosmarinic acid, a molecule that increases CB1 and CB2 activity, and which brings down neuroinflammation. 2
Because it works on both types of receptors, it is reasonable to expect that THC would work to restore the cytokine balance. But some people don’t want the psychoactivity, some people live in areas where using THC puts their job or their freedom at risk. If a person has chronic pain or epilepsy or muscle spasms, they might need something that works on the CB1 receptors on the nerves - in those cases, THC seems like the best tool. But if the issue is centered on the immune system and the CB2 receptors, a non-psychoactive option might be preferred.
Several other plants produce compounds that activate the CB2 receptor. Black pepper, cloves, and some citrus contain beta-caryophyllene, a terpenoid that is known to stimulate the CB2 receptors.3 And Echinacea and Spilanthes contain fairly selective CB2 receptor activators that seem to work the same way as AM1241.
Alkylamides and Anandamide
Echinacea and Spilanthes both produce alkylamides that are “selective CB2 receptor agonists.” Echinacea was used by Native Americans for cancer and inflammatory diseases. The most common modern western use of Echinacea is for colds and flu. Although Echinacea is often pitched for the ability to “strengthen the immune system,” it appears it actually works in the opposite way … it cools the immune system, it reduces inflammation.
The research that shows that Echinacea can shave a day or two off the back end of a cold seem to involve ending the fight against a microbe that has already been defeated. Many compounds go up in an active infection (histamine, interferons, TNF, etc, etc) and these make a person feel bad. Treatments that reduce these compounds allow the body to shift from a war-time footing to peace. The sirens in the body stop going off, things relax, and resources that were being directed to fighting now flow to normal body processes.
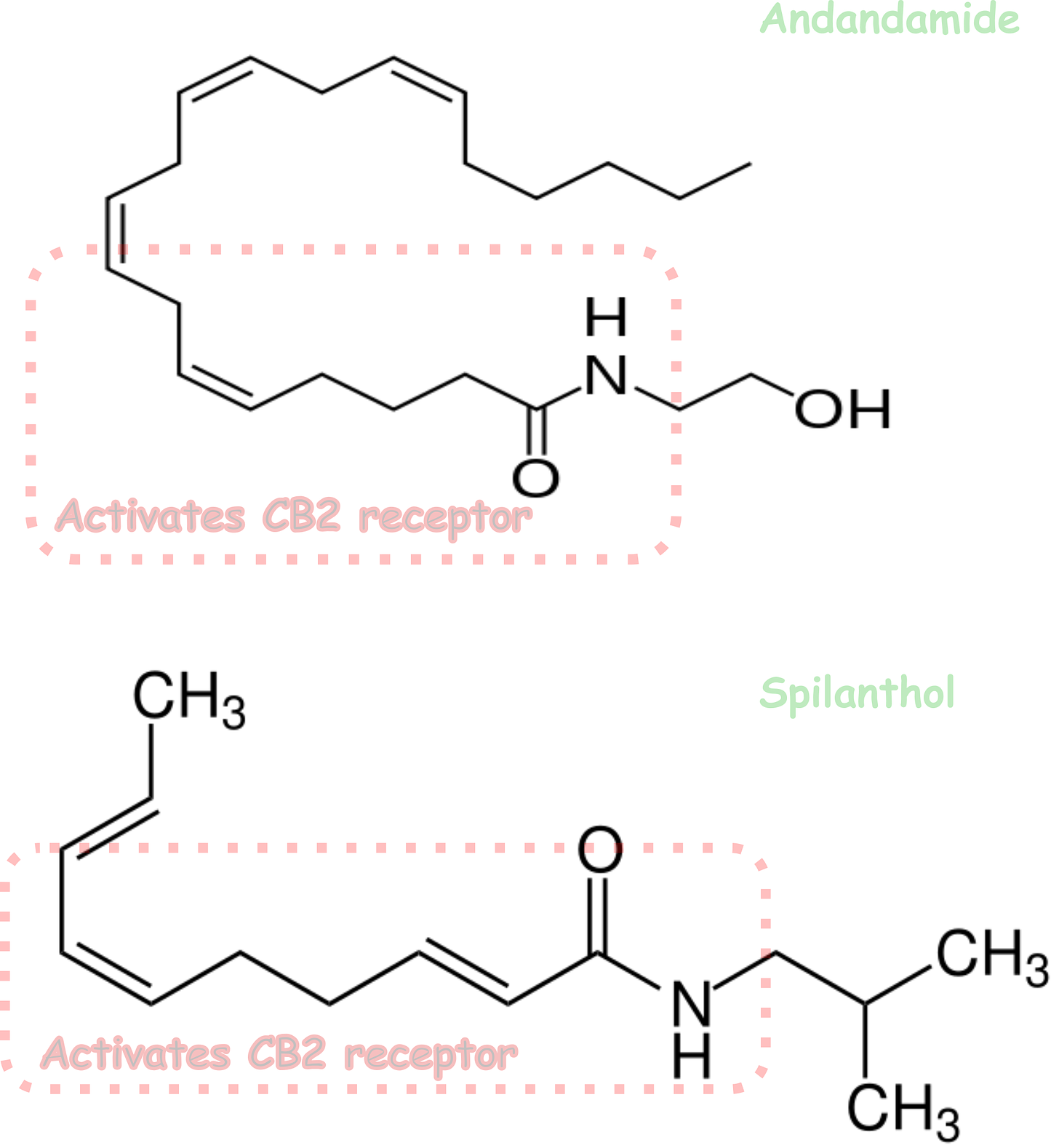
Alkylamides are basically fats that have a nitrogen/carbon/oxygen (amide) group attached to them. In our bodies, Anandamide is an important neurotransmitter - it is another fat that has an amide attached to it. Anandamide is the main endogenous molecule that activates the CB1 and CB2 receptors. THC works by mimicking anandamide - part of the THC molecule is similar enough to anandamide that it pushes the same buttons in the body. And so do the alkylamides in Echinacea and Spilanthes, although they are more selective and only push the CB2 buttons. But that may be all that is needed for some conditions.
Echinacea is widely available as a supplement, but I personally prefer the ‘Toothache Plant,’ Spilanthes acmella. Echinacea typically has to be grown 2 years or longer to get harvestable roots, but I can grow Spilanthes from seed to harvestable flowers in a few months, and get a continuous supply for daily use from a small pot filled with the ‘toothache plant.’ Spilanthes grows like a weed, and it is fast and easy to take cuttings from a mother plant to expand the grow.
Certainty
How sure are we that this mechanism results in meaningful improvement? Unfortunately, the certainty is still low. This mechanism has been shown to work in multiple animal studies, and there is a good chance it might work in people with long covid. The rationale is strong, the risks appear low - but the effectiveness hasn’t yet been verified. We don’t really know yet. Sorry to have to say ‘we don’t really know’ so often, but it is the truth. At this point, there is no proven therapy - our choices are to try something that is not fully proven, or do nothing. We are in a space where information is incomplete.
“Kavalactones and the endocannabinoid system: the plant-derived yangonin is a novel CB₁ receptor ligand.” Pharmacological Research, Aug 2012, PMID 22525682.
“Antidepressant-like effect of rosmarinic acid during LPS-induced neuroinflammatory model: The potential role of cannabinoid receptors/PPAR-γ signaling pathway.” Phytotherapy Research, Dec 2021, PMID 34709695.
“A mechanistic review on immunomodulatory effects of selective type two cannabinoid receptor β-caryophyllene.” Biofactors, 1 Jun 2022, PMID 35648433.